Need help?
[email protected]According to the CDC, 4.5 million Americans have chronic liver disease and almost 48,000 die from it each year.
From a coding and CDI perspective, chronic (or unspecified) liver failure is a non-CC and acute liver (hepatic) failure is classified as an MCC. How do we recognize chronic vs. acute liver failure? The table below illustrates the primary differences.
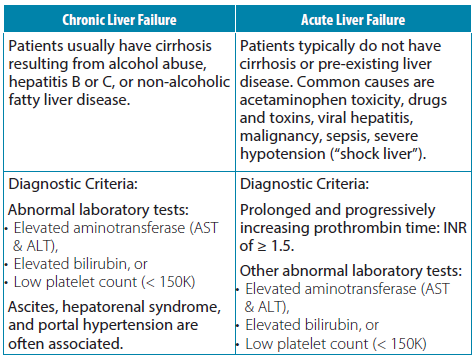
Other laboratory and clinical findings in liver failure include elevated creatinine, amylase/lipase, GGT, alkaline phosphatase, LDH; low pre-albumin/albumin; anemia. Physical findings include jaundice, hepatomegaly, RUQ/liver tenderness, ascites/edema, and asterixis (rhythmic “flapping” of hands when wrists held fully extended).
Get our CDI Pocket Guide® for more help with hepatic encephalopathy and failure.
What is hepatic encephalopathy? Patients with chronic liver failure are often admitted with hepatic encephalopathy which describes a spectrum of neurologic impairment. Symptoms include altered mental status, confusion, disorientation, inappropriate behavior, combativeness, gait disturbances, and/or altered level of consciousness ranging from drowsiness to deep coma. An elevated level of neurotoxic blood ammonia confirms the diagnosis, and it is treated with lactulose. Hepatic encephalopathy can be acute (overt), chronic, or acute on chronic.
From a coding perspective, hepatic encephalopathy does not have its own ICD-10 code and is indexed to “hepatic failure, not elsewhere classified” (category K72). When a patient is admitted with hepatic encephalopathy due to chronic liver cirrhosis, hepatic encephalopathy would be assigned as the principal diagnosis.
© 2022 Copyright Pinson & Tang LLC
Receive updates on new Resources, Products, and Events.
