Need help?
[email protected]Would you please explain the basics of the process from myocardial ischemia to injury to infarct? At what point does injury become an infarct?
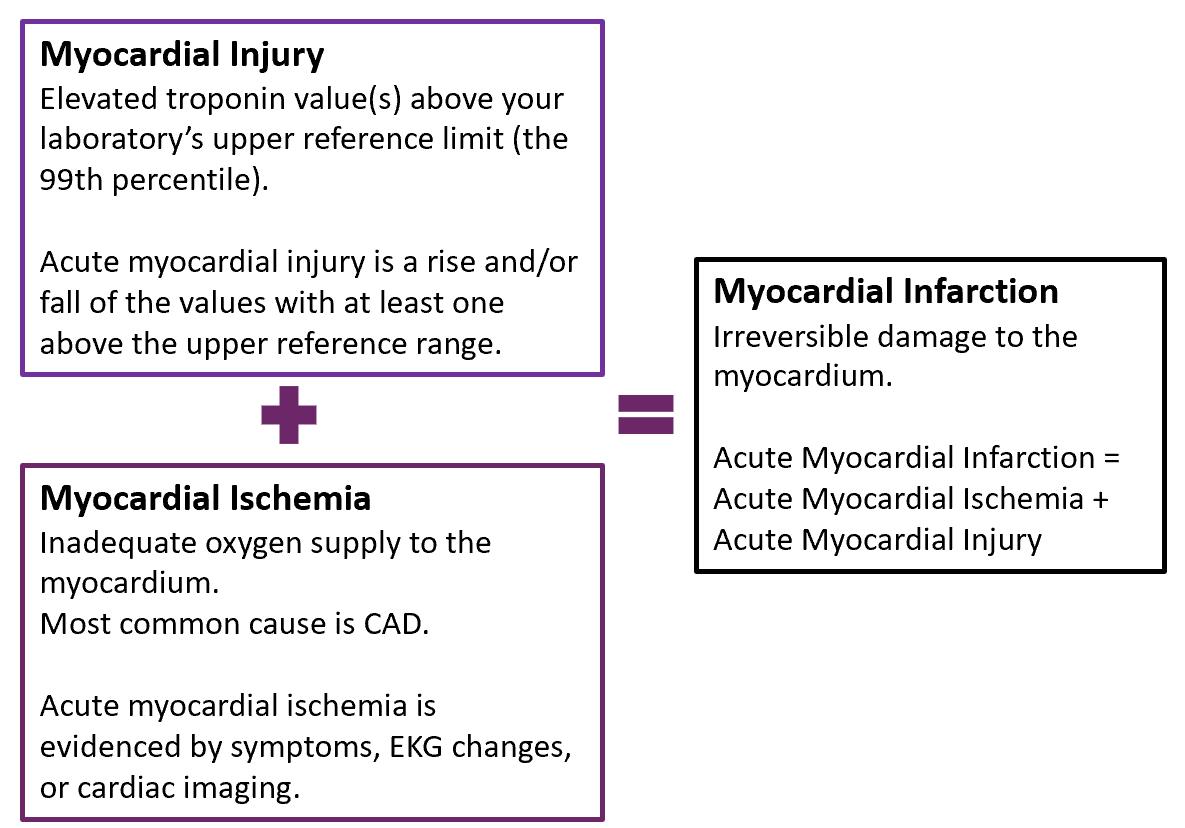
We'll start by defining myocardial ischemia, injury and infarction.
Myocardial ischemia simply means there is inadequate oxygen supply to the myocardium without damage to myocardial cells. No troponin is released in patients with chronic ischemia. The most common cause of ischemia is coronary artery disease (CAD). Patients who have CAD have chronically reduced oxygen supply to the myocardium putting them at risk for acute ischemia when oxygen demand exceeds oxygen supply, for example, when a person with CAD over-exerts causing angina.
Acute myocardial ischemia is evidenced by symptoms, EKG changes or cardiac imaging. If troponin is also released and above the 99th percentile (i.e., acute myocardial injury), a myocardial infarction has occurred. If not, then the patient only has unstable angina or demand ischemia.
Get our CDI Pocket Guide® to learn more about myocardial injury, ischemia, and infarction.
Myocardial injury is a new term introduced by the Fourth Universal Definition of Myocardial Infarction (2018). It is defined as an elevation of cardiac troponin values with at least one value above the 99th percentile upper reference limit (URL), often identified as a “critical value.”
Myocardial injury is considered acute when there is a rise and/or fall of troponin values, with at least one above the 99th percentile. When chronic, the troponin levels remain stable at a constantly elevated level. Myocardial injury may be due to ischemic or nonischemic causes.
To diagnose a myocardial infarction, the patient must have acute myocardial injury as well as evidence of acute myocardial ischemia (symptoms, EKG findings, imaging evidence).
Myocardial injury (acute or chronic) without evidence of acute myocardial ischemia is a non-MI troponin elevation secondary to a non-ischemic cause, i.e., non-ischemic myocardial injury. As of October 1, 2021, there is a new ICD-10 code I5A to capture the diagnosis of non-ischemic myocardial injury.
Myocardial Infarction is irreversible ischemic “injury” to the myocardium. An acute myocardial infarction occurs when acute myocardial ischemia causes myocardial injury. In other words, acute myocardial injury + acute myocardial ischemia = acute myocardial infarction.
Further details regarding evidence of acute myocardial ischemia, elevated troponin levels (myocardial injury), and ischemic vs. non-ischemic causes of myocardial injury are provided below.
For a diagnosis of acute myocardial infarction there must be evidence of acute myocardial ischemia. There are three ways you could look for evidence of myocardial ischemia: (1) symptoms, (2) new EKG changes and (3) imaging evidence.
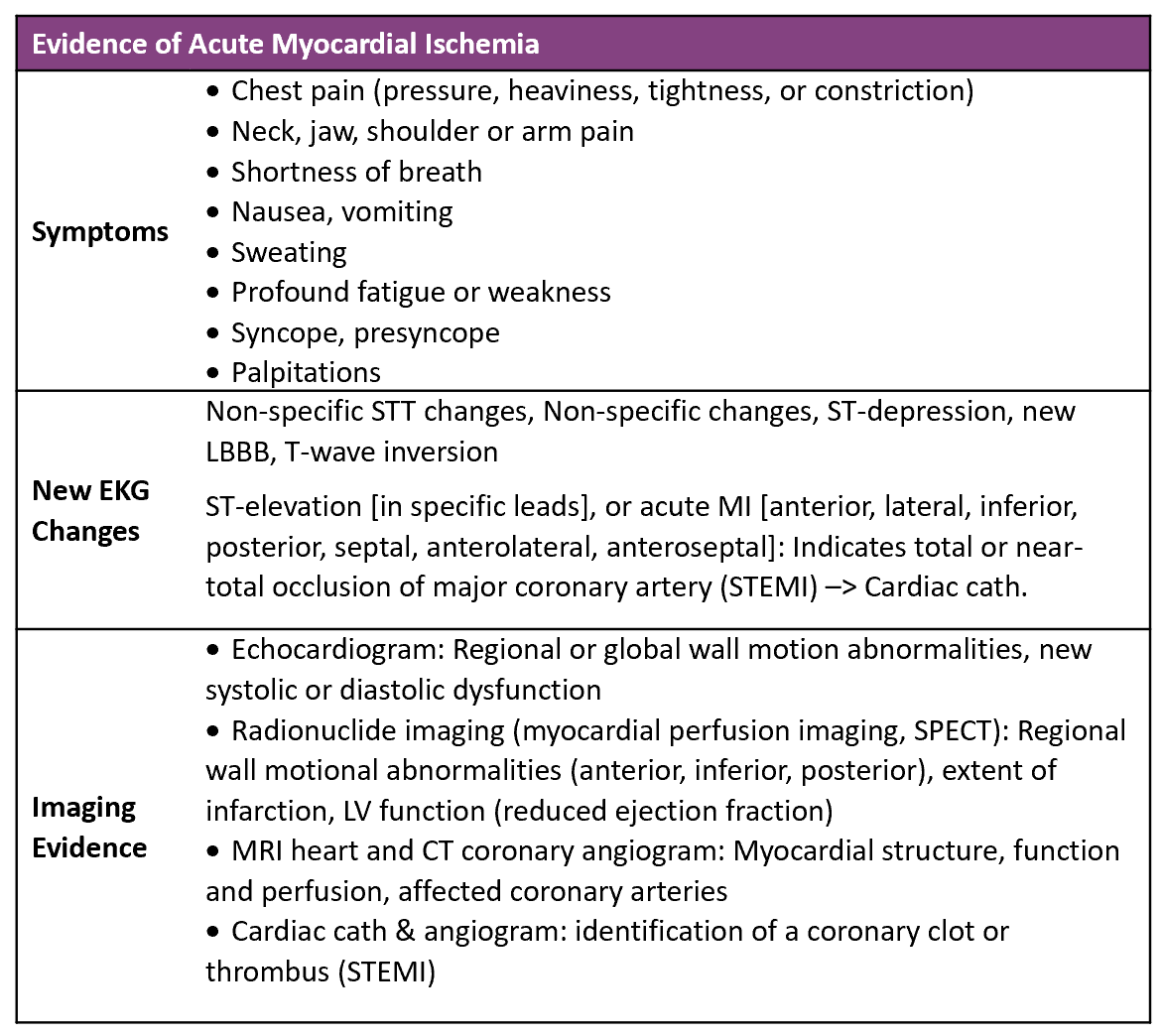
Symptoms. The symptoms of ischemia are also those that are often consistent with an acute coronary syndrome or myocardial infarction. But they're not just chest pain, pressure, heaviness, tightness. There are many things that may be associated with myocardial ischemia that we may not think of. Most of us are familiar with the chest pain with radiation to neck, jaw, shoulder or arm, which is usually on the left side. Sometimes there's an epigastric location, but that may be difficult to separate from the substernal location and may accompany it. Shortness of breath, nausea, vomiting, sweating are not unusual. Some people only express a sense of profound fatigue or weakness. Syncope or presyncope can be the only symptom, and that's usually due to some type of an arrhythmia associated with an ischemic myocardium.
New EKG changes. The above table is intended to list things you may actually see on the EKG report or that may be described by the physicians when they're talking about the EKG and evidence of ischemia such as nonspecific STT changes, or nonspecific STT-wave changes, or “nonspecific changes”, or ST-depression, or new left bundle branch block, new Q-waves, or T-wave inversion
ST elevation is characteristic of STEMI and the EKG may say ST elevation in certain specific leads, like leads 2,3 and aVF, or 1 and aVL or V1-V3. Alternatively, the location of the MI may be stated like inferior, lateral or anterior.
Cardiac Imaging. Imaging evidence includes echocardiogram, the radioactive nuclide imaging (myocardial perfusion), or SPECT. MRI of the heart and CT angiograms, or cardiac cath with angiography, and other modalities can identify wall motion abnormalities, systolic or diastolic dysfunction, changes in ejection fraction. Extent of infarct is sometimes identified as well as structural abnormalities, perfusion abnormalities of affected coronary arteries and with cardiac cath intracoronary thrombus may be identified.
Troponin levels in suspected myocardial infarction are measured on admission, typically two to four hours after admission, six to eight hours after admission for the third, and occasionally a fourth measurement at 12 hours depending on whether the first three are diagnostic or not. Troponin I is preferred to troponin T because it's a little more specific and a bit more accurate.
In general, higher troponin levels are associated with more extensive myocardial injury. Peak troponin values are usually highest in STEMIs, then NSTEMIs, and lowest overall in non-ischemic (non-MI) causes. Keep in mind though that a very high troponin level alone is not diagnostic of a myocardial infarction and must be supported by evidence of acute myocardial ischemia.
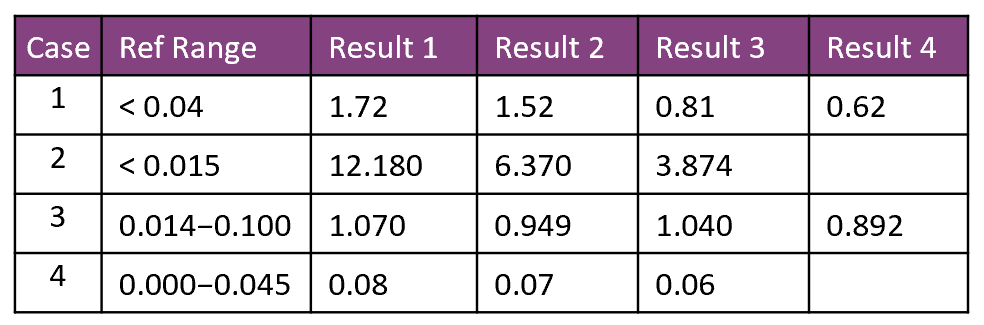
In Case #1, there is evidence of acute myocardial injury because the troponin level is very high compared to the URL of 0.04 and it falls from 1.72 to 0.62. If there is also evidence of acute myocardial ischemia (symptoms, new EKG changes, cardiac imaging), we have an acute myocardial infarction either Type 1 or Type 2, depending on the cause.
The same is true for Case #2 where there is a dramatic fall from a very high level of 12.180 to 3.874, compared to the upper reference limit of 0.015. Elevated troponin levels of this magnitude are often associated with a STEMI.
In Case #3, the troponin level is elevated but there is a slight fall and then a slight rise occurs followed by another fall that is more or less stable without a clear trend. This likely represents chronic nonischemic myocardial injury.
Case #4 shows only very slightly elevated levels and are rather flat. We don't really know if they are dropping. These might be within the normal range for this patient even though these are above the normal reference range.
How quickly does the troponin level disappear after injury? It can take up to two weeks for the troponin level to return to normal, so a delayed diagnosis of myocardial infarction can still be made.

The above table shows the ischemic and other nonischemic causes of myocardial injury. Ischemic causes of myocardial injury in the setting of acute myocardial ischemia are myocardial infarctions of all types, most commonly Types 1 and 2. The causes of Type 2 MI are non-CAD causes and included above.
If the cause of the myocardial injury is non-ischemic, there is no myocardial infarction. It's important to recognize that patients with heart failure, cardiac procedures, infections, critical illness, kidney disease, CVA and many other noncoronary causes can have elevated troponin levels, but without an ischemic cause, there is no myocardial infarction. Do not query for a myocardial infarction unless there is evidence of acute myocardial ischemia.
This is not to say that patients with these conditions cannot also have acute myocardial ischemia, such as the patient with both heart failure and CAD. Do not query for a myocardial infarction unless there is evidence of acute myocardial ischemia.
Myocardial injury is defined as an elevation of cardiac troponin values with at least one value above the 99th percentile upper reference limit. Acute myocardial injury is when there is a rise and/or fall of the troponin levels. Myocardial injury can be either acute or chronic and due to ischemic (CAD) or non-ischemic causes.
There are multiple causes of nonischemic myocardial injury that are both cardiac and noncardiac. A new ICD-10 code I5A has been created for non-ischemic myocardial injury.
Acute myocardial ischemia is identified by symptoms, new EKG changes, and/or cardiac imaging.
Acute myocardial infarction (AMI) is acute myocardial injury in the setting of acute myocardial ischemia. Myocardial infarction is ischemic myocardial injury.
(c) 2021 Pinson & Tang.
Receive updates on new Resources, Products, and Events.
